Abstract
Background
Obesity can negatively affect pulmonary function tests, with or without clinical symptoms, but the impact of bariatric weight loss is still debated. Aiming to document such profile in a consecutive homogeneous population, a prospective cohort study was undertaken.
Methods
Sixty-one patients (100% females, age 40 ± 8 years, BMI 49 ± 5 kg/m2 and without respiratory disease) were enrolled. Spirometric analysis was carried out to compare preoperative respiratory pattern with outcome after 6 and 12 months. Variables included vital capacity (VC), expiratory reserve volume (ERV), forced expiratory volume (1 s) (FEV1), FEV1/FVC ratio and maximum voluntary ventilation (MVV). Correlation of results with weight loss was examined.
Results
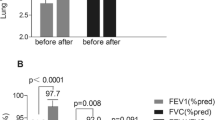
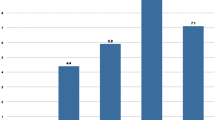
The following initial variables exhibited significant difference when compared to the 12-month postoperative control: FVC (P = 0.0308), FEV1/FVC (P = 0.1998), MVV (P = 0.0004) and ERV (P = 0.2124). Recovery of FVC and FEV1/FVC occurred earlier by 6 months. The most seriously depressed preoperative finding was ERV, which even after 1 year still remained inadequate.
Conclusions
(1) Pulmonary limitations were diagnosed in approximately one third of the population. (2) Changes were demonstrated for FVC, FEV1/FVC, ERV and MVV. (3) FEV1 and FEV1/FVC were acceptable due to the absence of an obstructive pattern. (4) Two variables increased by 6 months (FEV1/FVC and ERV), whereas recovery for others was confirmed after 1 year. (5) The only exception was ERV which continued below the acceptable range.


Similar content being viewed by others
References
Biring MS, Lewis MI, Liu JT, et al. Pulmonary physiologic changes of morbid obesity. Am J Med Sci. 1999;318:293–7.
Bottai M, Pistelli F, Di Pede F, et al. Longitudinal changes of body mass index, spirometry and diffusion in a general population. Eur Respir J. 2002;20:665–73.
Chen Y, Rennie D, Cormier YF, et al. Waist circumference is associated with pulmonary function in normal-weight, overweight, and obese subjects. Am J Clin Nutr. 2007;85:35–9.
Crapo RO, Kelly TM, Elliott CG, et al. Spirometry as a preoperative screening test in morbidly obese patients. Surgery. 1986;99:763–8.
Hakala K, Maasilta P, Sovijarvi AR. Upright body position and weight loss improve respiratory mechanics and daytime oxygenation in obese patients with obstructive sleep apnoea. Clin Physiol. 2000;20:50–5.
Hankinson JL, Odencrantz JR, Fedan KB. Spirometric reference values from a sample of the general U.S. population. Am J Respir Crit Care Med. 1999;159:179–87.
Collins LC, Hoberty PD, Walker JF, et al. The effect of body fat distribution on pulmonary function tests. Chest. 1995;107:1298–302.
Lazarus R, Sparrow D, Weiss ST. Effects of obesity and fat distribution on ventilatory function: the normative aging study. Chest. 1997;111:891–8.
Koenig SM. Pulmonary complications of obesity: a review. Am J Med Sci. 2001;321:249–79.
Rasslan Z, Saad Junior R, Stirbulov R, et al. Evaluation of pulmonary function in class and II obesity I. Bras Pneumol. 2004;30:508–14.
Hansen JE, Sun XG, Wasserman K. Spirometric criteria for airway obstruction: use percentage of FEV1/FVC ratio below the fifth percentile, not <70%. Chest. 2007;131:349–55.
Zavorsky GS, Kim DJ, Sylvestre JL, et al. Alveolar-membrane diffusing capacity improves in the morbidly obese after bariatric surgery. Obes Surg. 2008;18:256–63.
Catheline JM, Bihan H, le Quang T, et al. Preoperative cardiac and pulmonary assessment in bariatric surgery. Obes Surg. 2008;18:271–7.
Collet F, Mallart A, Bervar JF, et al. Physiologic correlates of dyspnea in patients with morbid obesity. Int J Obes (Lond). 2007;31:700–6.
Jones RL, Nzekwu MM. The effects of body mass index on lung volumes. Chest. 2006;130:827–33.
Acknowledgement
This study was supported by a post-doctorate FAPESP grant number 06/51197-5. The valuable help of Prof. Antonio C. Valezi is appreciated.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Souza, S.A.F., Faintuch, J. & Cecconello, I. Spirometric Function Improves in the Morbidly Obese After 1-Year Post-surgery. OBES SURG 20, 1273–1277 (2010). https://doi.org/10.1007/s11695-010-0142-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-010-0142-y